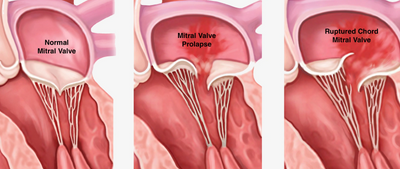
Mitral regurgitation (MR) is a condition in which the heart's mitral valve leaflets do not coapt (close) tightly. This allows some blood to flow backward into the left atrium (upper heart chamber), rather than through the aorta to the rest of the body. If the regurgitation is significant, the patient may feel tired or out of breath due to decreased efficiency of the heart. Treatment of MR depends on its severity.
It also depends on whether the patient experiences symptoms or the condition is worsening.
For mild leakage, treatment is usually not necessary. Severe leakage or regurgitation may call for surgical intervention to repair or replace the dysfunctional valve. Left untreated, it can cause heart failure or arrhythmias. Even patients without symptoms may require evaluation by a cardiologist and trained surgeon to determine whether early intervention may be beneficial.
Symptoms
Symptoms of mitral valve disease may not be experience for many years. Signs and symptoms of MR, which depend on its severity and progression, can include:
- Heart murmur (abnormal heart sound)
- Dyspnea (shortness of breath)
- Fatigue
- Heart palpitations (rapid, fluttering heartbeat)
- Swollen feet or ankles
MR is often mild and progresses slowly. However, the problem may develops quickly, and a sudden onset of severe signs and symptoms can occur.
Causes
Primary MR is caused by problems with the valve, itself. Diseases of the left ventricle can lead to secondary or functional MV regurgitation.
Possible causes of MR include:
- Mitral Valve prolapse → leaflets bulge back into the left atrium during the heart's contraction.
- Ischemia → inadequate blood flow can cause dimensional changes in the heart, which dilates the ring of the valve and prevents the leaflets from fully coapting.
- Damaged tissue cords → over time, the chordae tendinae (tissue cords) that anchor the flaps of the mitral valve to the heart wall may stretch or tear, especially in patients suffering from MV prolapse.
- Rheumatic fever → A complication of untreated strep throat can damage the mitral valve, leading to regurgitation early or later in life.
- Endocarditis → An infection of the lining of the heart (endocarditis) can involve the MV.
- Heart attack → Damage to the area of the heart muscle that supports the MV, can affect its function.
- Cardiomyopathy (abnormality of the heart muscle) → Over time, the heart's accommodation of certain conditions, such as high blood pressure, can gradually enlarging the left ventricle and stretch the tissue around the mitral valve.
- Trauma → trauma can cause physical damage leading to MR.
- Congenital heart defects → some babies are born with defects in their hearts, including damaged heart valves.
- Certain drugs → prolonged use of certain medications , such as those containing ergotamine (Cafergot, Migergot), can lead to MR.
- Radiation therapy → In rare cases, radiation therapy for cancer can lead to MR.
Risk Factors
Several factors can increase a patient's of mitral valve regurgitation, such as:
- History of mitral valve prolapse or stenosis → Having either condition does not necessarily guarantee MR; a family history of valve disease also can increase risk of MR.
- Heart attack → A heart attack can cause damage that affects the function of the mitral valve.
- Heart disease → Coronary artery disease, for example, can lead to MR.
- Certain medications → Drugs containing ergotamine (Cafergot, Migergot) lead to an increased risk of mitral regurgitation.
- Infections such as endocarditis or rheumatic fever → Infections or the inflammation they cause can damage the mitral valve.
- Congenital heart disease → Some individuals are born with an abnormal valve that is prone to regurgitation.
- Age → By middle age, natural deterioration may lead to MR.
Minimally Invasive Treatment Options
<< Heart Diseases
Minimally Invasive Procedures >>